MGCP Survey demonstrates a growing community confidence in biomedical HIV prevention strategies
[et_pb_section admin_label=”section”][et_pb_row admin_label=”row”][et_pb_column type=”4_4″][et_pb_text admin_label=”Text” background_layout=”light” text_orientation=”left” use_border_color=”off” border_color=”#ffffff” border_style=”solid”]
Media Release
[/et_pb_text][et_pb_divider admin_label=”Divider” color=”#ffffff” show_divider=”on” divider_style=”solid” divider_position=”top” hide_on_mobile=”on” height=”5″] [/et_pb_divider][et_pb_text admin_label=”Text” background_layout=”light” text_orientation=”left” use_border_color=”off” border_color=”#ffffff” border_style=”solid”]
The results of this year’s Melbourne Gay Community Periodic Survey demonstrate a growing community confidence in the efficacy of biomedical HIV prevention strategies amongst gay men and other men who have sex with men (MSM). This includes a nearly threefold increase in the uptake of pre-exposure prophylaxis (PrEP) and over 97% of men living with HIV on treatment having achieved an undetectable viral load (UVL). The 2017 results also recorded the highest ever level of HIV testing which has increased over time to 90% of men in the survey – continuing the upward trend over the last several years.
Conducted by the Centre for Social Research in Health at UNSW, the 2017 survey captured the responses of 2,956 gay men and other MSM to a broad set of questions related to sex, relationships and sexual health.
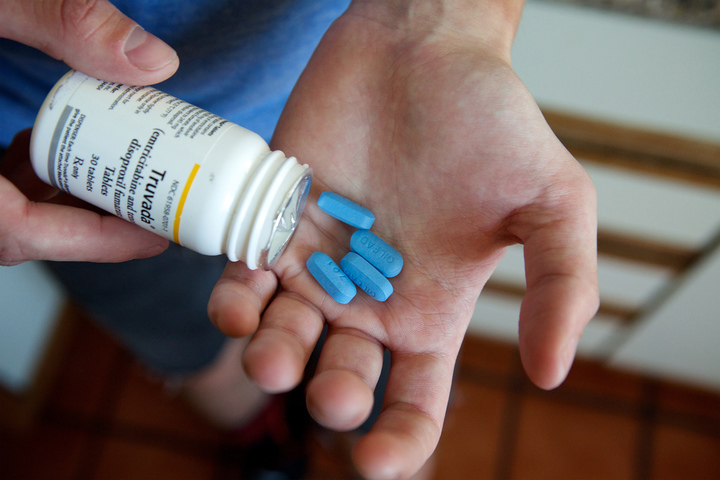
The proportion of men using PrEP increased from 6% in 2016 to 16% in 2017, with most of the men on PrEP in the 2017 survey (84%) obtaining it from a research study or trial. In Victoria, PrEP has been made available through the PrEP-X study, sponsored by the Victorian Government, Alfred Health, and the Victorian AIDS Council (VAC).
VAC CEO Simon Ruth said that these findings add momentum to prevention efforts across the community.
“This is further evidence that when it comes to HIV prevention, gay men are at the forefront in protecting themselves and others. When taken consistently, PrEP is proven to be close to 99% effective at preventing HIV.”
“What we need now is for the Commonwealth to list PrEP on the Pharmaceutical Benefits Scheme as soon as is possible to ensure all people at risk of HIV can benefit.”
Over 99% of men living with HIV in the survey reported being on HIV treatment and over 97% of those men in treatment having an undetectable viral load – meaning they are not infectious and cannot pass on HIV.
“HIV positive men are playing a substantial role in the low rates of new HIV infections by working to maintain an undetectable viral load,” said Brent Allan, CEO of Living Positive Victoria.
“There is increasing evidence that UVL amongst men living with HIV will be a key factor in the decline of new diagnoses in Australia.”
The majority (87.7%) of HIV positive men who have condomless sex with casual partners reported UVL as their primary risk reduction strategy.
“Biomedical HIV prevention tools mean that safe, condomless sex is possible; however, PrEP and UVL won’t protect people from other STIs so it’s important that sexually active men test regularly to maintain their sexual health and wellbeing,” Mr Ruth said.
The 2017 survey results around testing are encouraging with 77% of men testing for HIV in the previous 12 months (the highest level recorded in the survey) and an increase in the proportion of men reporting 3 or more HIV tests in the previous year (30% in 2017). Over 92% of men living with HIV reported an STI test in the previous 12 months, and STI testing amongst HIV negative men is continuing to rise with nearly 78% having tested in the past 12 months.
Click here for the full media release
Infographic of Melbourne Gay Community Periodic Survey
[/et_pb_text][/et_pb_column][/et_pb_row][/et_pb_section]